13 March 2026
Everything you need to know about HSCT for your child — explained clearly, step by step.
Table of Contents
Hearing that your child needs a hematopoietic stem cell transplant (HSCT) — commonly known as a Bone Marrow Transplant (BMT) — can be overwhelming for any parent. This recommendation often comes after several medical consultations and treatments. However, advances in pediatric hematology and oncology have made HSCT one of the most effective curative treatments for several serious childhood diseases. This guide explains the process, indications, risks, and expectations of pediatric stem cell transplant in simple language so parents can understand and prepare for the journey ahead.
What Is a Hematopoietic Stem Cell Transplant (HSCT)?
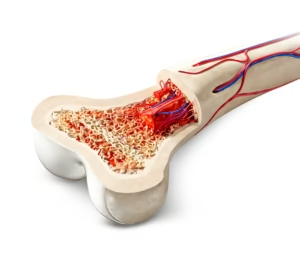
A hematopoietic stem cell transplant (HSCT) is a medical procedure in which unhealthy or damaged bone marrow is replaced with healthy stem cells. These stem cells settle inside the bone marrow and begin producing normal blood cells.
Bone marrow is responsible for making three critical types of blood cells:
RED BLOOD CELLS
Carry oxygen throughout the body to keep organs and tissues healthy.
WHITE BLOOD CELLS
Form the body’s immune defence, fighting bacteria, viruses, and infections.
PLATELETS
Help the blood clot properly, preventing excessive bleeding after injury.
When the bone marrow fails or begins producing abnormal cells, a transplant can help restore normal blood formation and, in many cases, cure the underlying disease entirely.
When Is Pediatric Stem Cell Transplant Recommended?
HSCT may be recommended for several serious childhood conditions. Understanding your child’s diagnosis is the first step toward knowing whether a transplant is the right path forward.
BLOOD CANCERS
Leukemia and lymphoma may require transplant when the disease is high-risk or returns after initial treatment.
BONE MARROW FAILURE
Aplastic anemia occurs when the marrow stops producing blood cells altogether
INHERITED BLOOD DISORDERS
Conditions like thalassemia major and sickle cell disease can often be cured through transplant.
IMMUNODEFICIENCY
Some children are born with weak immune systems; transplant replaces the defective immune system with a healthy one.
Types of Pediatric Stem Cell Transplant
There are two main types of stem cell transplant used in children, and the right choice depends on the underlying condition and the availability of a suitable donor.
ALLOGENEIC TRANSPLANT
Stem cells come from a donor. The donor may be a matched sibling, an unrelated donor from international registries, a half-matched parent (haploidentical transplant), or umbilical cord blood.
AUTOLOGOUS TRANSPLANT
Stem cells come from the child’s own body. These cells are collected before intensive chemotherapy and infused
back after treatment is complete.
The Step-by-Step Transplant Process
Pediatric stem cell transplant follows a carefully structured sequence. Each phase is monitored closely by a specialised transplant team.
Pre-Transplant Evaluation
Doctors perform blood tests, bone marrow examination, and organ function tests to ensure the child is fit for transplant.
Donor Search
Siblings are checked first for HLA matching. If no match is found, unrelated donor registries or parent donors (haploidentical) may be considered.
Conditioning Therapy
Chemotherapy — and sometimes radiation — is administered to destroy diseased cells and prepare the body to accept the new stem cells.
Stem Cell Infusion
Healthy stem cells are infused through a central line — similar to a blood transfusion. This is the transplant itself.
Engraftment
The new stem cells settle in the bone marrow and begin producing healthy blood cells, usually within 10–28 days after infusion.
Hospital Stay and Recovery
Recovery from a pediatric stem cell transplant takes place in stages — beginning in the hospital and continuing at home over several months. Here is what to expect at each phase:
DURING HOSPITALISATION (3–5 WEEKS)
Most children remain in hospital for approximately 3–5 weeks after transplant. Doctors closely monitor blood counts, check for infections, and manage any complications during this critical window.
AFTER DISCHARGE (SEVERAL MONTHS)
Regular follow-up visits are required for several months after discharge, while the immune system gradually recovers. Children need infection precautions, balanced nutrition, and scheduled vaccinations.
RETURN TO NORMAL LIFE (6–12 MONTHS)
Most children gradually return to school and normal daily activities within 6–12 months after transplant, as their immune system strengthens and recovery progresses.
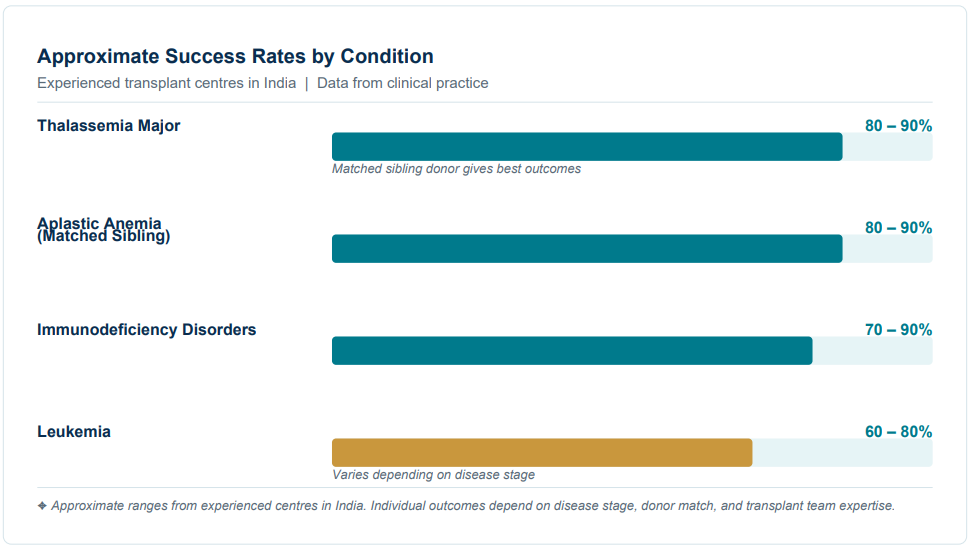
Success Rates of Pediatric Stem Cell Transplant in India
HSCT outcomes have improved greatly over the past two decades. In experienced transplant centres across India, success rates are encouraging across a range of conditions. Early diagnosis and treatment at experienced transplant centres significantly improve the chances of success.
Risks of Stem Cell Transplant in Children
Although a pediatric stem cell transplant can be life-saving, it is a complex treatment that carries potential risks.
Transplant teams are trained to detect and manage these problems early, and most complications can be treated effectively when identified in time.
POSSIBLE RISKS TO BE AWARE OF
- Infections due to low immunity
- Graft-versus-Host Disease (GVHD)
- Delayed recovery of blood counts
- Organ complications
These risks are actively monitored throughout the transplant journey. The specialised transplant team works continuously to prevent complications and respond to any that arise.
Life After Pediatric Stem Cell Transplant
Recovery continues for several months after leaving the hospital. While this period requires patience and care, most children go on to lead healthy, active lives. Here is what to keep in mind during the recovery phase:
INFECTION PRECAUTIONS
Careful hygiene and avoiding crowded spaces protects the child while the immune system rebuilds.
BALANCED NUTRITION
A healthy, well-balanced diet supports recovery, energy, and immune function.
FOLLOW-UP VISITS
Regular outpatient appointments track blood counts and immune recovery over several months.
VACCINATIONS
The transplant resets immunity, so children require a fresh vaccination schedule post-transplant.
Most children gradually return to school and normal activities within 6–12 months after transplant. While each child’s timeline differs, the goal — and in most cases, the outcome — is a return to a full and normal life.
Frequently Asked Questions
Success rates vary depending on the disease but are generally between 70–90% in experienced transplant
centres. Conditions like thalassemia major and aplastic anemia (with a matched sibling donor) see rates of 80–90%, while leukemia outcomes range from 60–80% depending on disease stage.
Yes. A matched sibling donor is often the best option and typically provides excellent outcomes. Siblings are
always the first to be tested for HLA compatibility.
Most children remain in hospital for approximately 3–5 weeks after transplant, depending on the pace of recovery and any complications that need managing.
Possible risks include infections (due to low immunity during recovery), graft-versus-host disease (GVHD), delayed blood count recovery, and organ complications. These are monitored closely by the transplant team and can usually be managed effectively.